Introduction: What Do Patients Mean by “Puffy Nipples”?
“Puffy nipples” is a non-medical, umbrella term commonly used by men to describe a fullness, bulge, or projection within the nipple–areola complex.
Importantly, this description does not represent a single diagnosis. The underlying cause can vary significantly from one patient to another, and in many cases, more than one factor may be present.
From a clinical perspective, the key principle is this:
The treatment must be tailored to the cause — not the label.
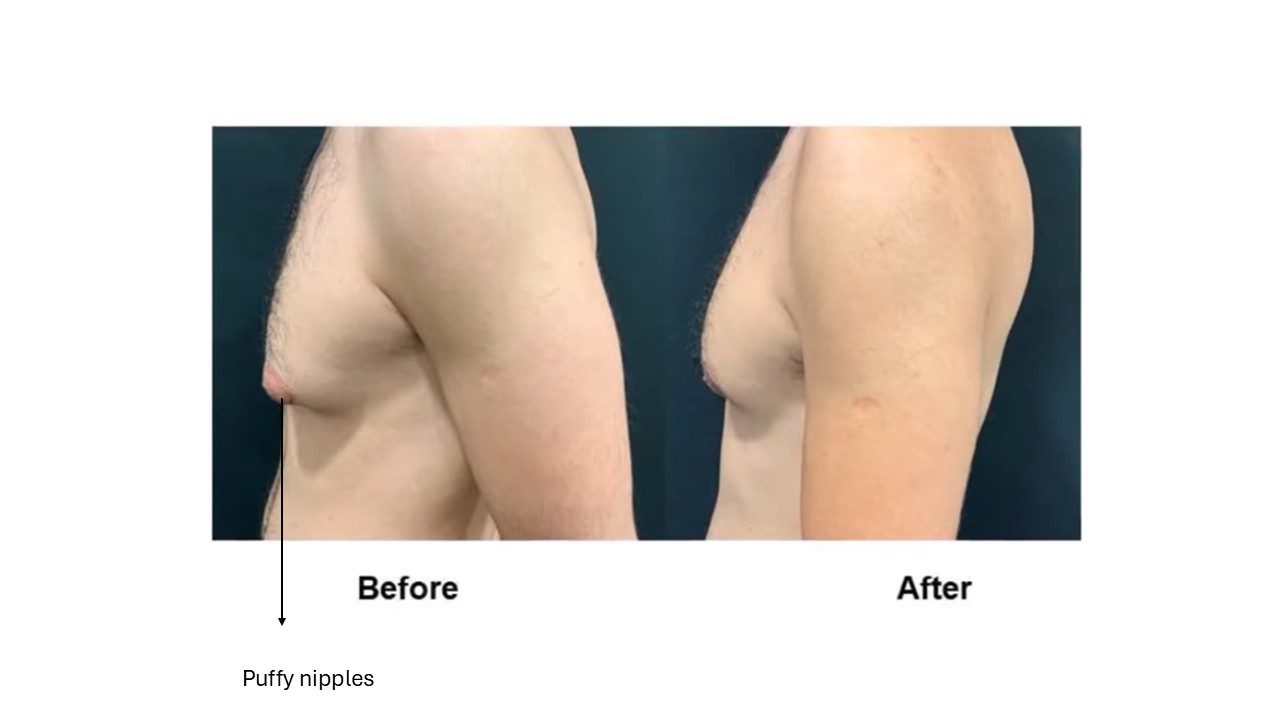
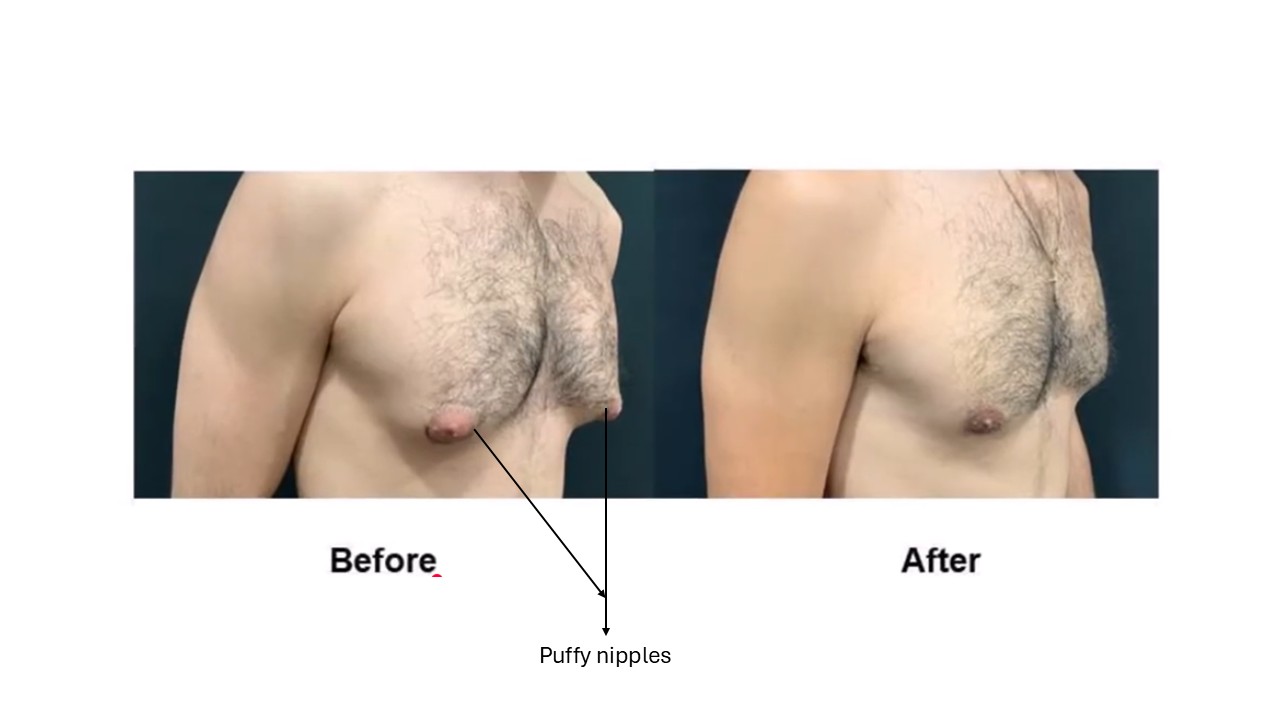
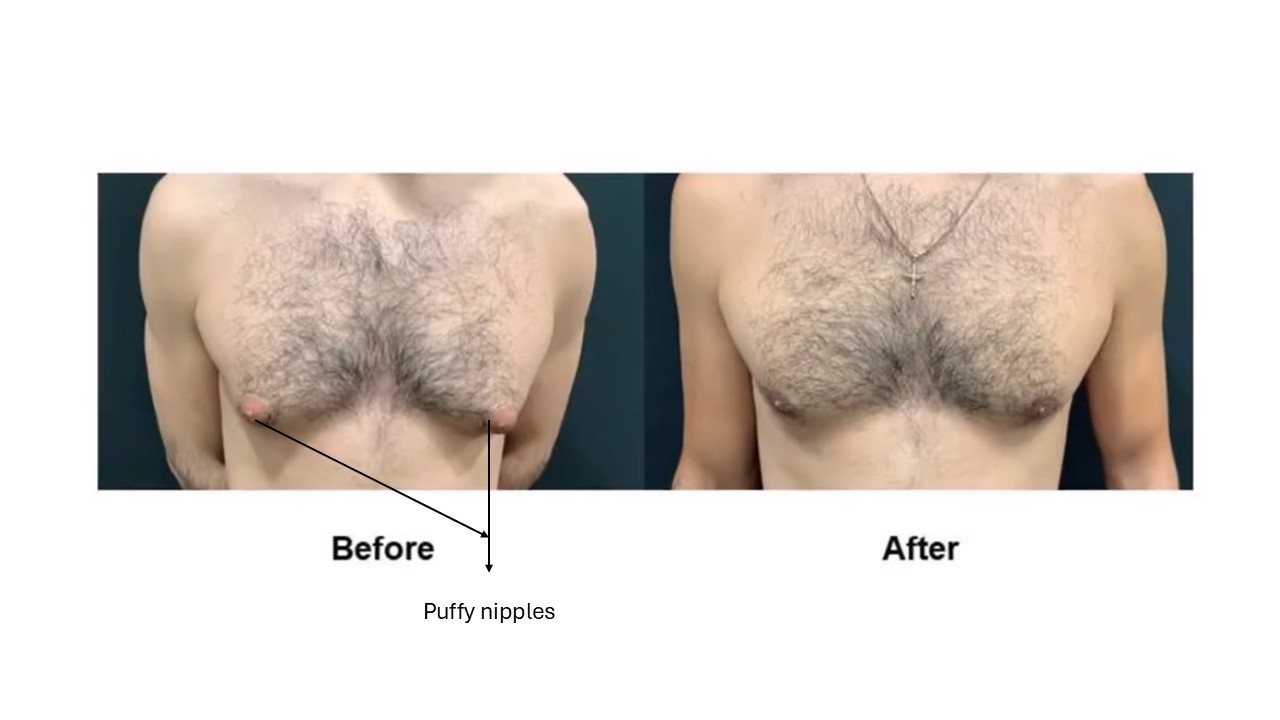
Is Puffy Nipple a Medical Problem?
In the vast majority of cases, puffy nipples are:
- Benign
- Bilateral
- Not harmful
- Not associated with cancer or serious disease
- Any significant pathology needs to be excluded by medical practitioners.
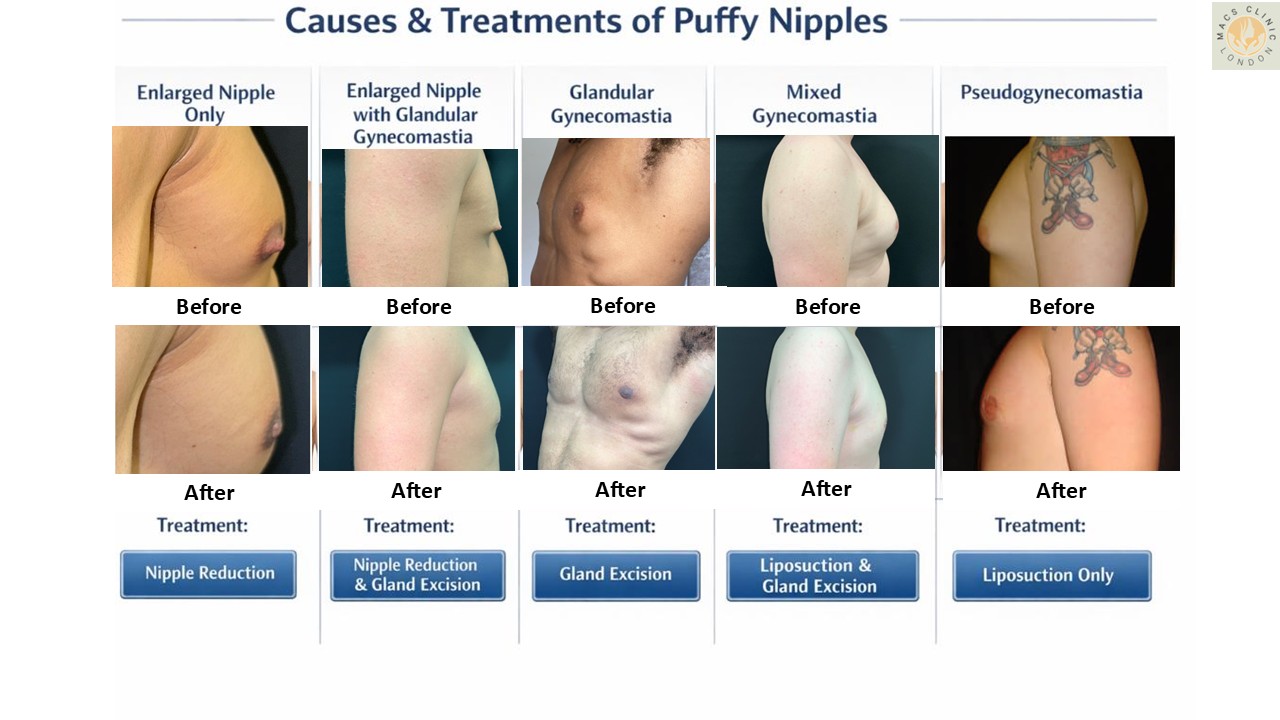
Common Causes of Puffy Nipples
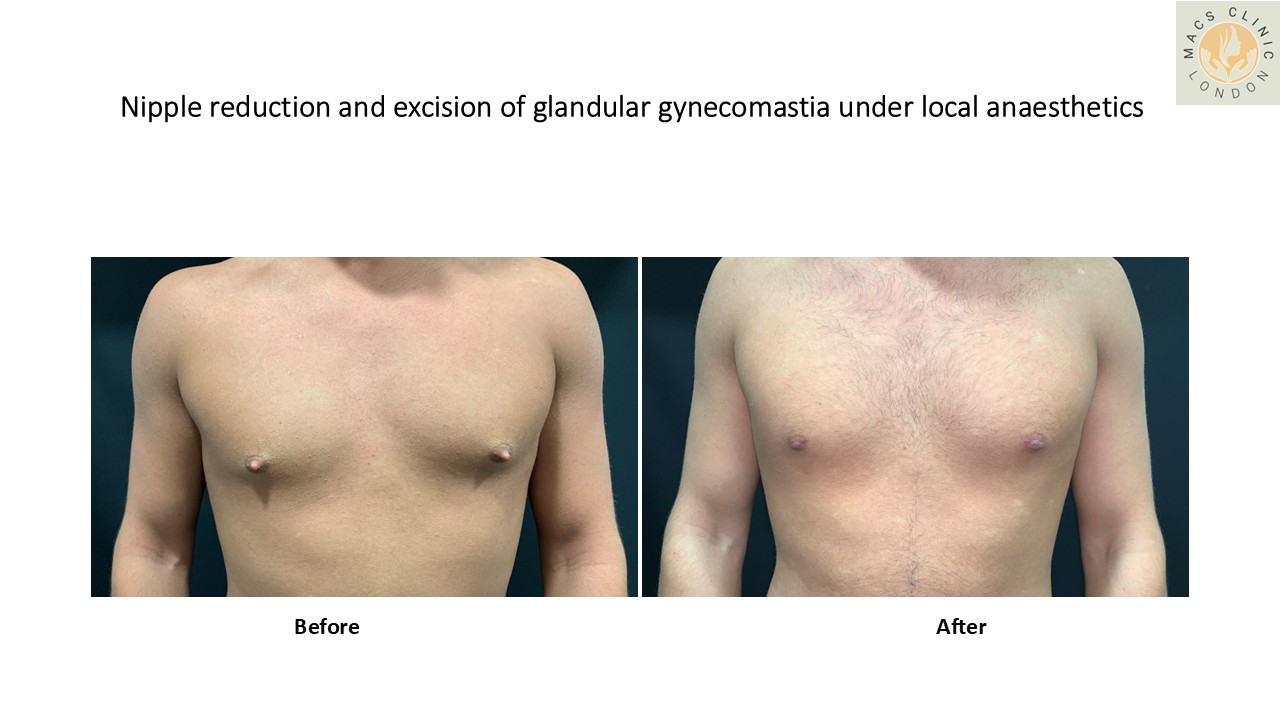
- Glandular Gynecomastia
This is true gynecomastia caused by an overgrowth of breast gland tissue beneath the nipple–areola complex.
Clinical features:
- Firm or rubbery tissue under the nipple
- Increased nipple projection
- Sometimes tender and painful
- Often bilateral, occasionally asymmetric
They are therefore considered a non-essential cosmetic concern, provided rare underlying conditions have been excluded.
Causes:
Hormonal imbalance (often physiological), medications, anabolic steroids, or idiopathic (no identifiable cause).
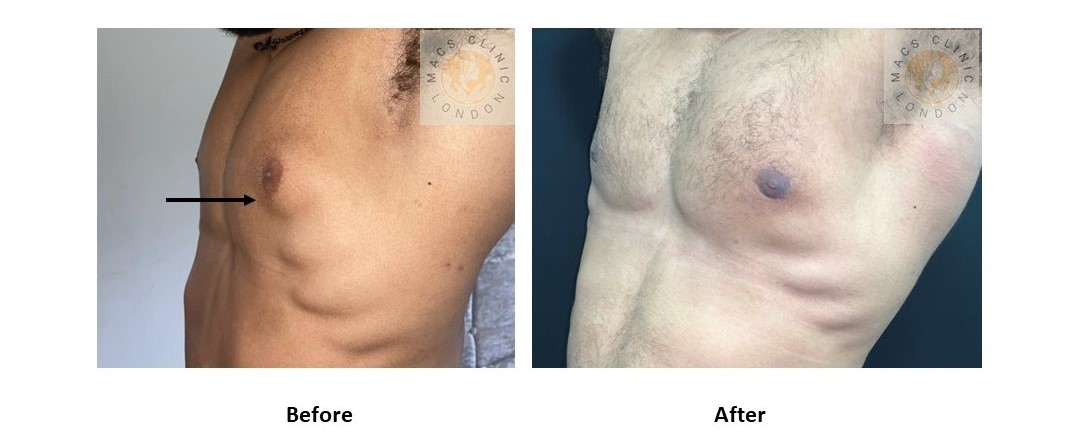
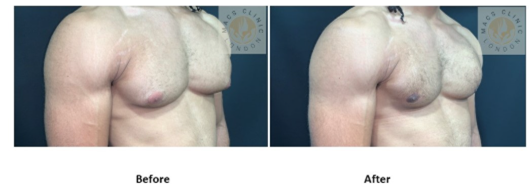
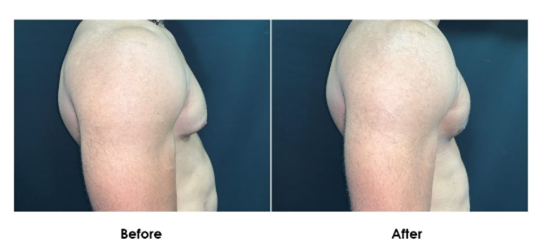
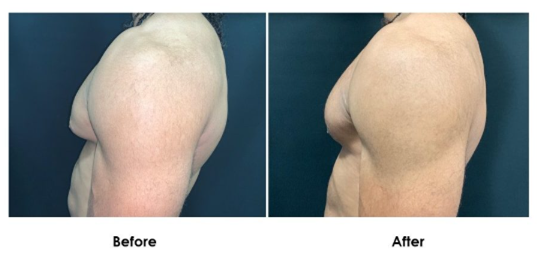
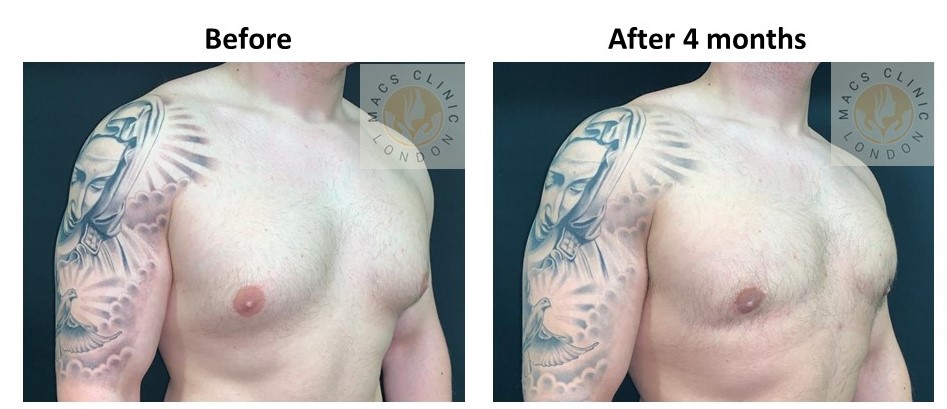
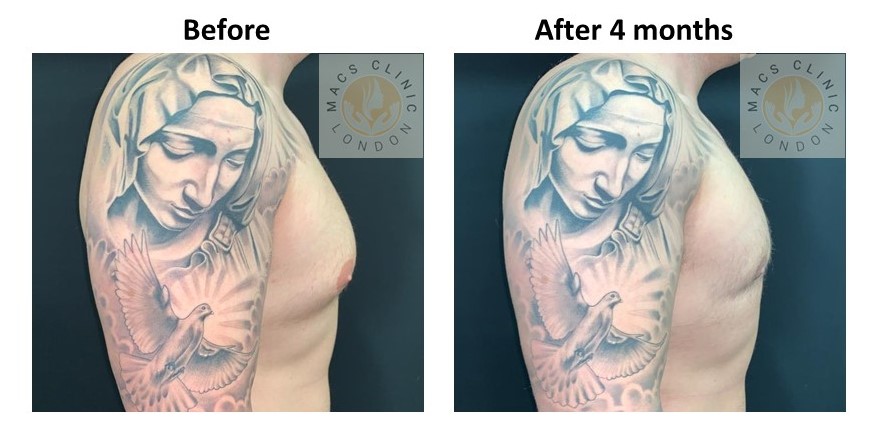
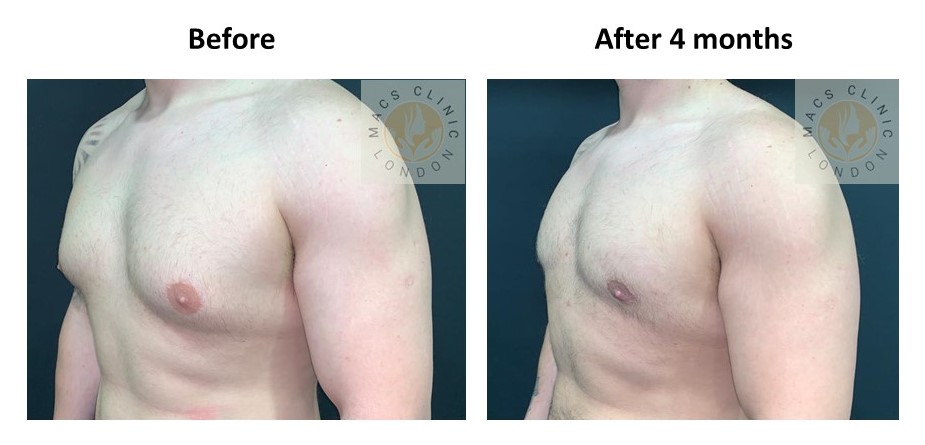
2. Mixed Gynecomastia (Gland + Fat)
A combination of:
- Glandular tissue
- Surrounding fatty tissue
This is very common and often seen in men with normal or mildly elevated body fat.
Clinical features:
- Puffy nipple with broader chest fullness
- Soft fat with a firmer core beneath the nipple
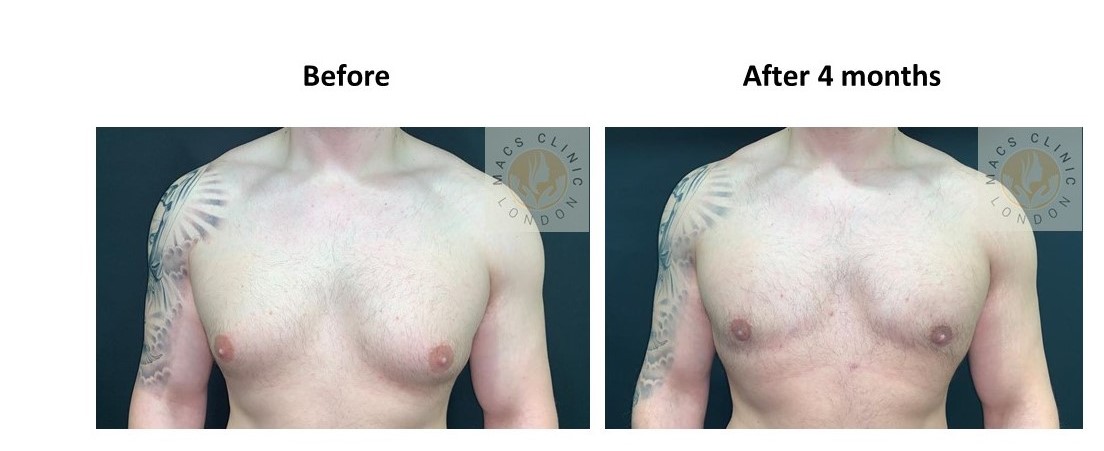
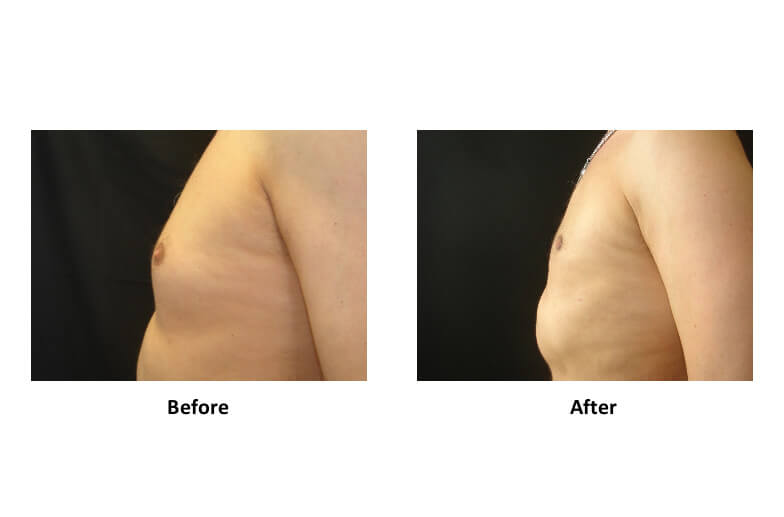
- Pseudogynecomastia (Fat-Predominant) –
This is not true gynecomastia.
Cause:
- Excess fatty tissue alone
- No glandular enlargement
Clinical features:
- Soft, compressible fullness
- Puffy appearance improves when lying flat
- Often associated with weight gain and obesity
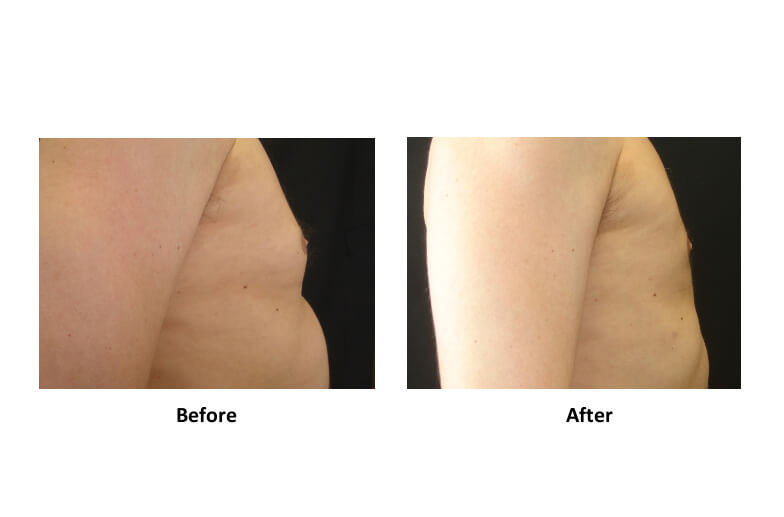
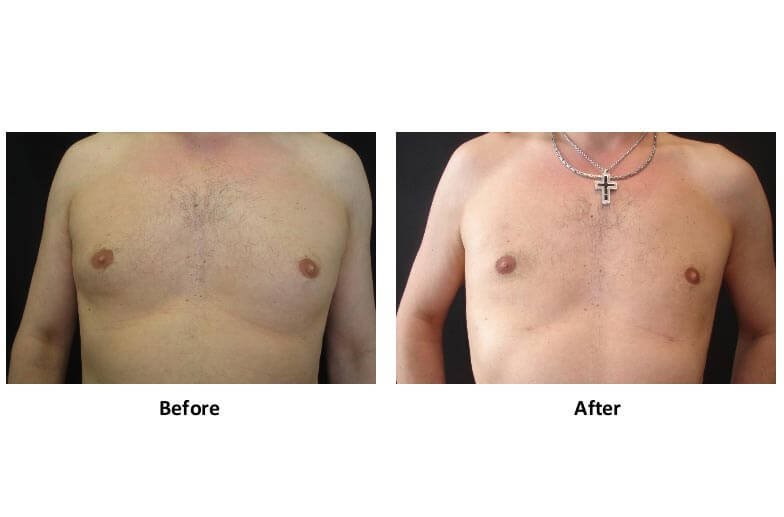
- Prominent Nipple Without Gynecomastia
Some men naturally have:
- Increased nipple projection
- No underlying gland or fat excess
This is a normal anatomical variation, not a disease.
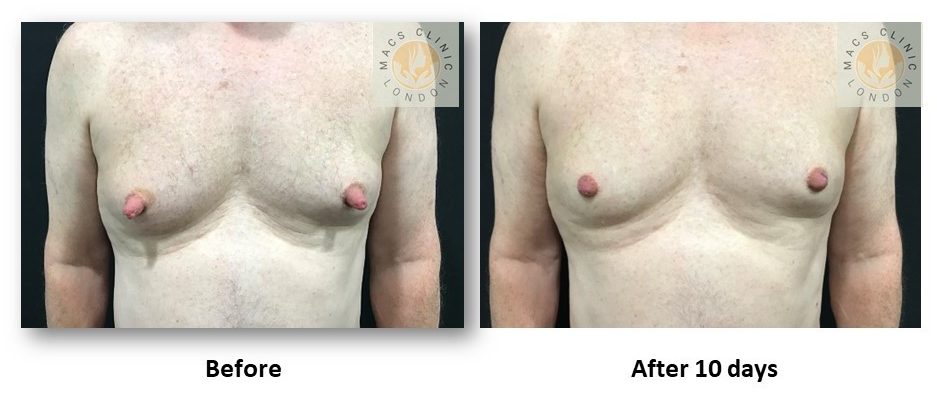
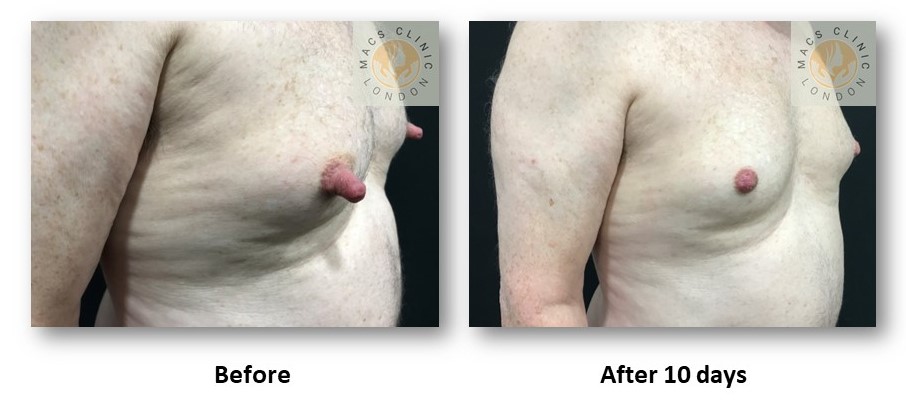
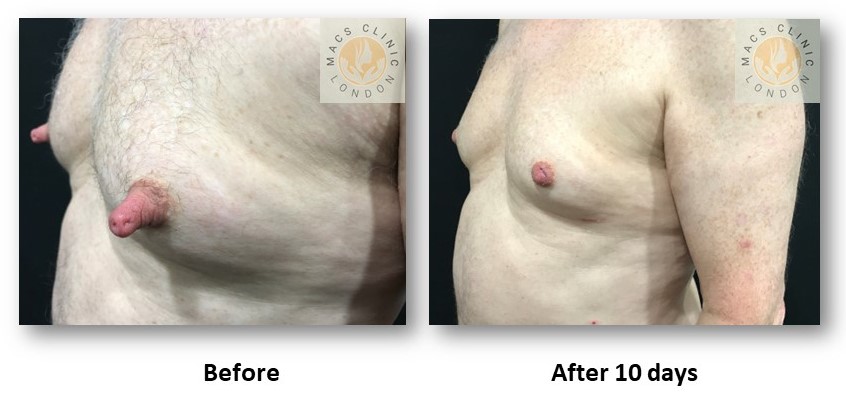
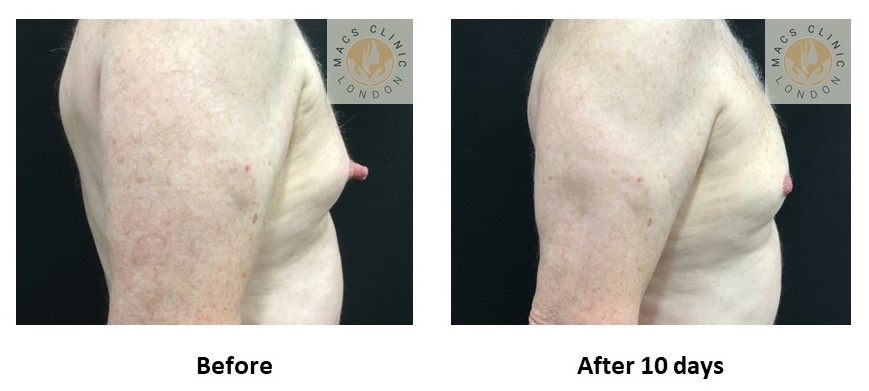
- Combination Patterns (Very Common)
Many patients have more than one contributing factor, such as:
- Prominent nipple + glandular gynecomastia
- Large areola + fat bulge
- Nipple projection + mixed gynecomastia
This is where careful assessment becomes essential.
The Professional Dilemma with surgical implications
A frequent and important scenario in practice:
The patient consults for nipple prominence,
but the surgeon detects underlying gynecomastia that the patient has not noticed or complained about.
This raises an ethical responsibility:
- It is advisable that the medical practitioner should refrain from medicalising or magnifying patient’s concerns and insecurities.
- The medical practitioners should avoid creating New insecurities
- The consultation must remain patient-centred, proportionate, and transparent
At MACS Clinic, this is addressed by:
- Focusing first on the patient’s stated concern
- Explaining findings factually and neutrally
- Clearly documenting what is and is not being treated
- Ensuring consent is specific, comprehensive
- and realistic
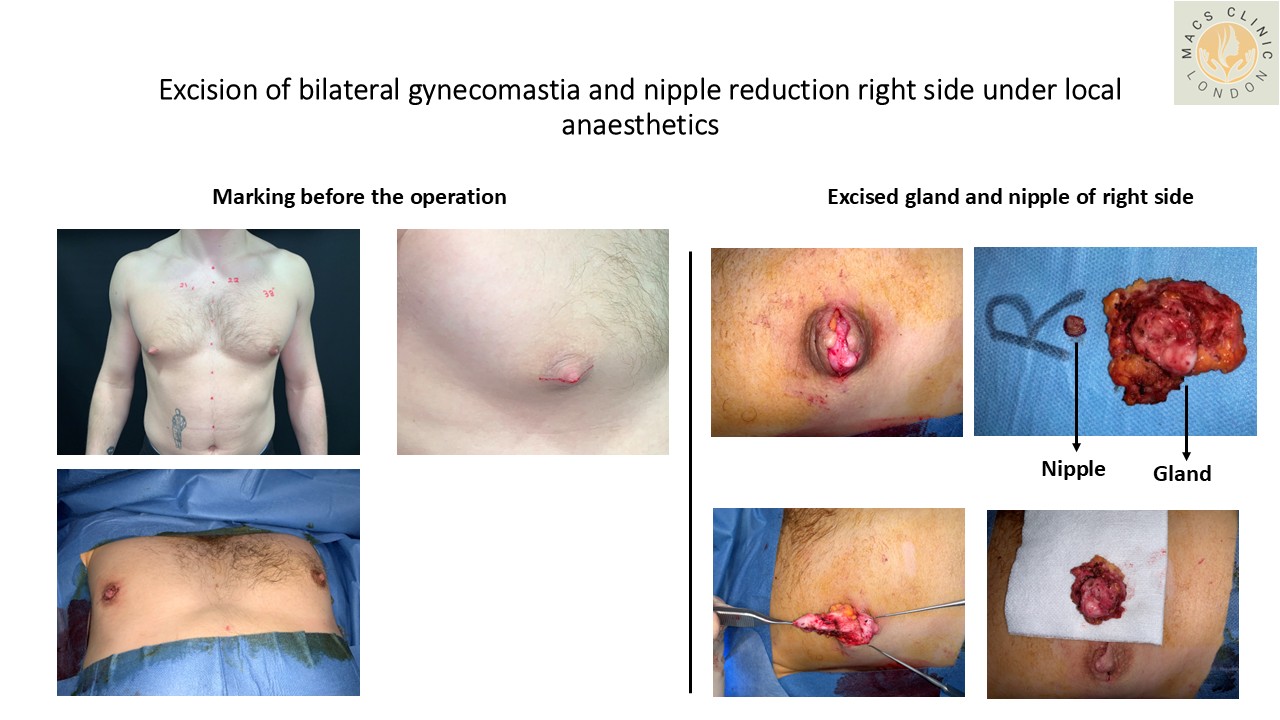
Investigations: When Are They Needed?
Investigations should be considered if:
- Rapid or unilateral enlargement
- Pain, discharge, or skin changes
- Significant asymmetry
- Relevant drug or endocrine history
Possible investigations:
- Ultrasound/MRI scan
- Hormonal blood tests
- GP and endocrinology referral
Surgical Treatment Options – Targeted to the Cause
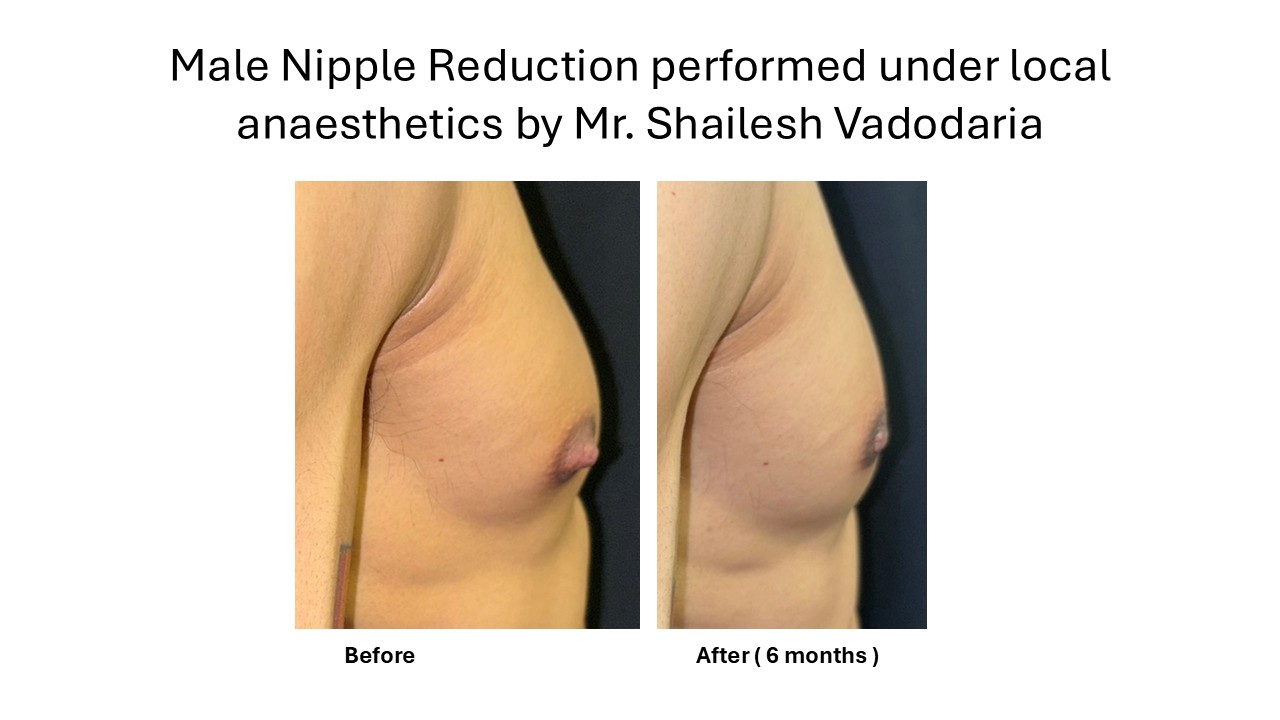
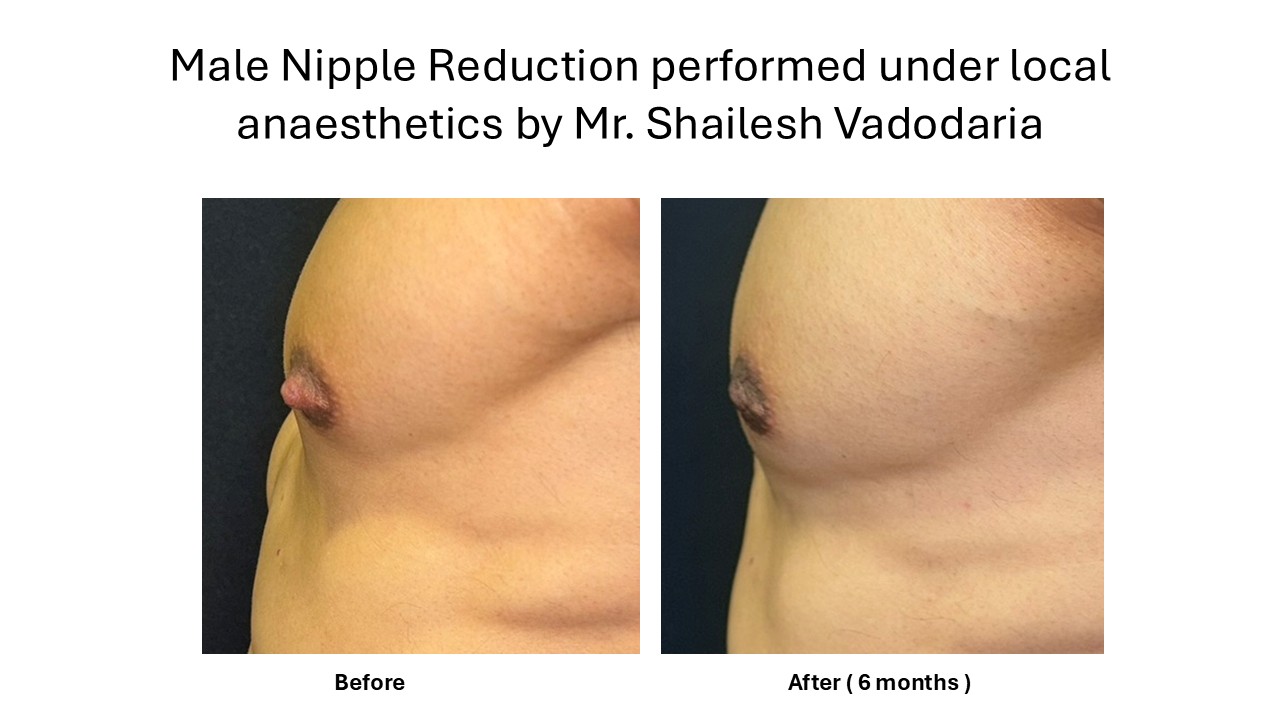
- Nipple Reduction Surgery
Indicated when:
- Primary issue is excess nipple projection
- Minimal or no gland/fat excess
At MACS Clinic:
- Performed under local anaesthesia as a day case procedure
- Precise reduction using published, peer-reviewed techniques
- Minimal scarring
⚠️ Important consent point:
This procedure addresses nipple height only, not underlying chest fullness unless specifically planned.
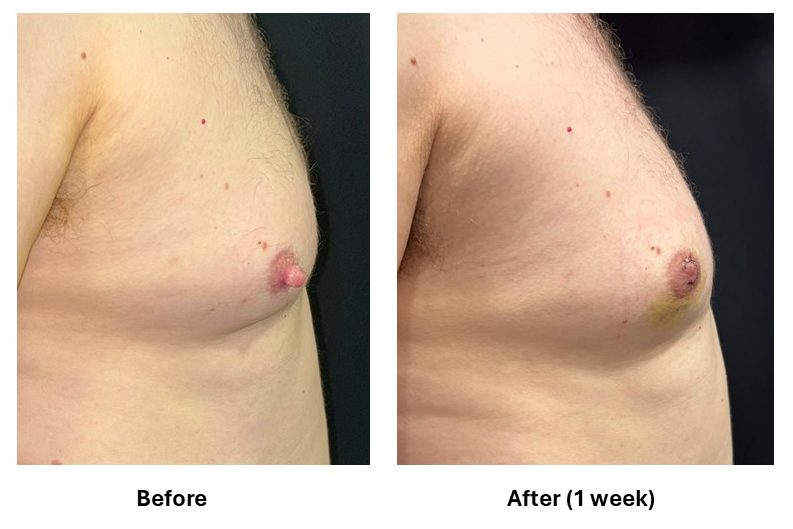
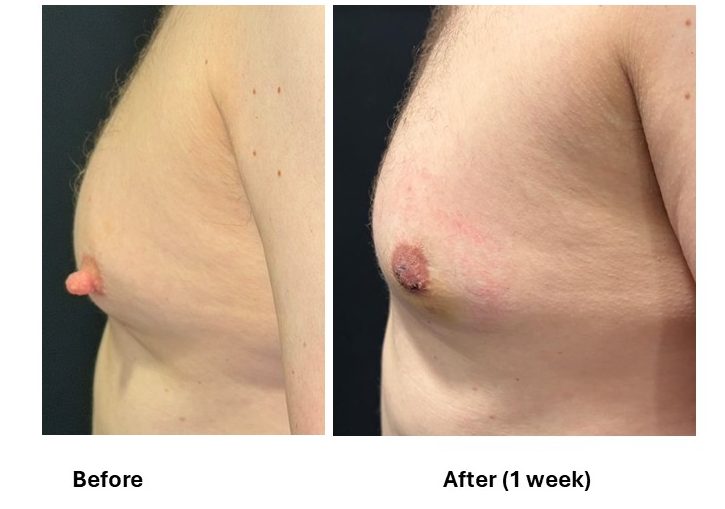
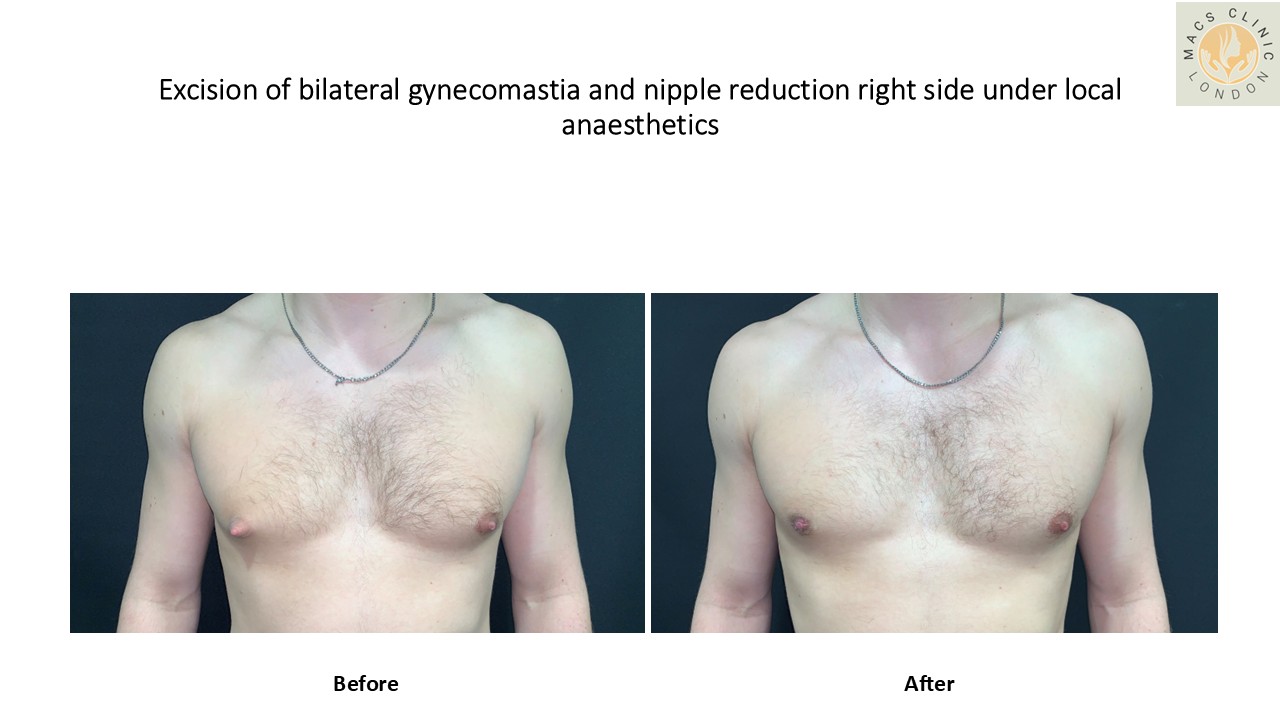
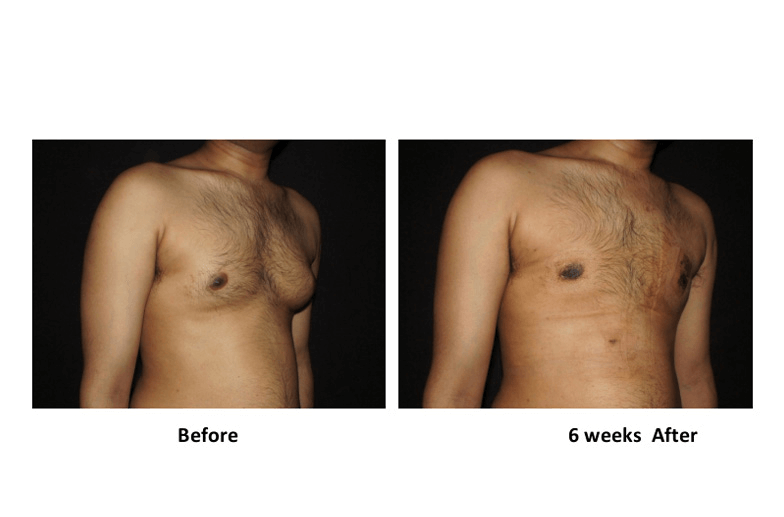
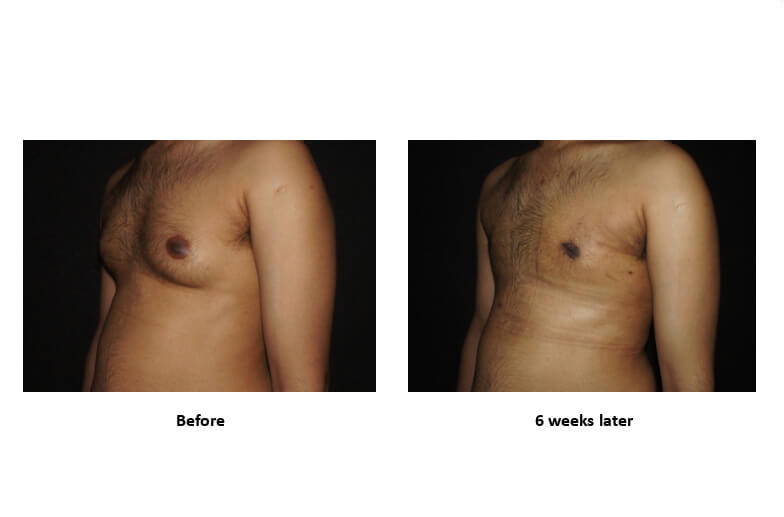
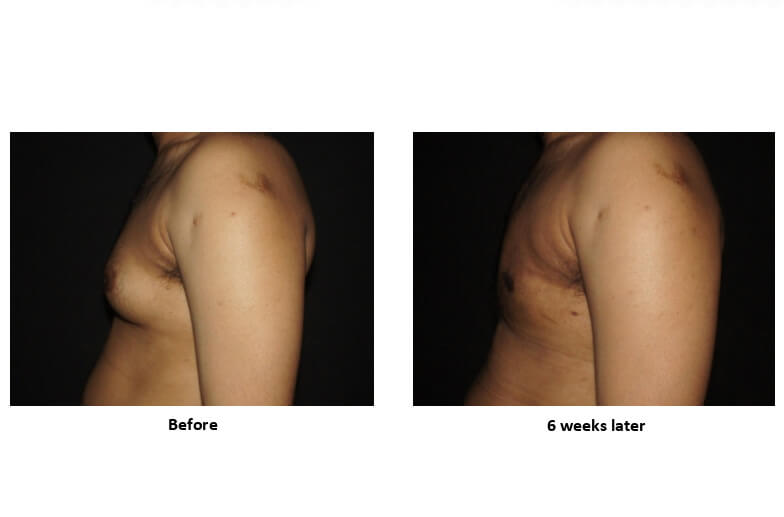
- Liposuction-Assisted Gynecomastia Surgery
Indicated for:
- Mixed gynecomastia
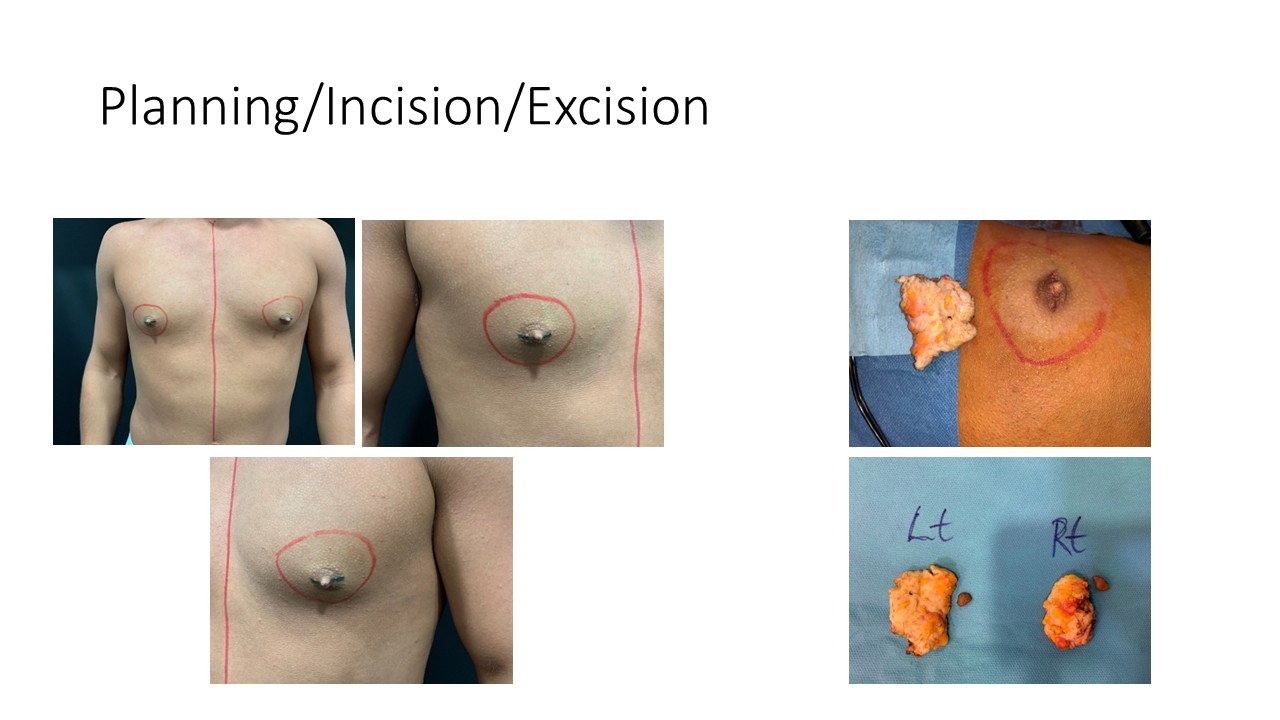
Technique:
- Liposuction to contour fat
- Targeted removal of fibrofatty through a cut within the nipple areola complex
- Improves chest contour and nipple puffiness
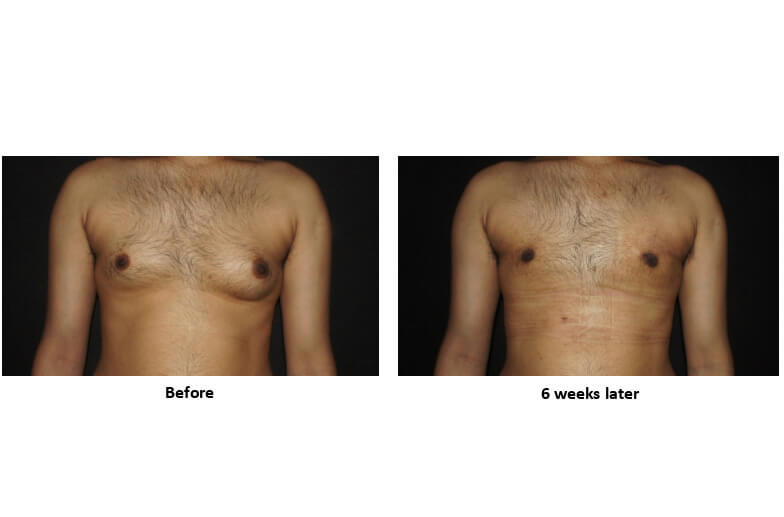
- Liposuction Alone
Indicated for:
- Pseudogynecomastia (fat-only)
Benefits:
- No gland excision required
- Less invasive
- Puffy nipple often resolves as fat is reduced
Patients are advised to lose weight and develop chest wall muscle mass.
Key Messages for Patients
- “Puffy nipples” is a descriptive term, not a diagnosis
- There are multiple causes, often in combination
- Treatment should be individualised and proportionate
- Surgery is only required if patients are self-conscious
- When surgery is chosen, it is cosmetic, optional, and carefully consented
Summary
Puffy nipples in men are common, benign, and usually multifactorial.
A thoughtful and evidence-based approach ensures:
- Accurate diagnosis
- Targeted treatment
Our patients request for correction of puffy nipples for following reasons –
- It affects their self-esteem
- Not comfortable using tight and light t-shirts
- Affects their confidence in using swimming pool, common changing room and compromises enjoying beach holidays
We have started seeing many more patients developing puffy nipples because of consumption of steroids/testosterone for body building.
At MACS Cosmetic Surgery, the guiding principle is simple:
Treat the concern the patient has come with —
and only extend treatment when it is appropriate, requested, and fully understood.
Contact MACS Clinic
- Phone: 020 7078 4378
- WhatsApp: 07792 648 726
- Email: enquiries@macsclinic.co.uk
- Website: www.macsclinic.co.uk
BOOK a FREE Video Consultation: https://calendly.com/macsclinic/free-video-consultation?month=2025-01






